The Arrive Trial: Labor Induction versus Expectant Management in Low-Risk Nulliparous Women (1)
Clinical Question: Does induction of labor at 39 weeks of gestation result in a lower risk of a composite outcome of perinatal death or severe neonatal complications compared to expectant management among low-risk, nulliparous women?
Journal: New England Journal of Medicine
Publication date: August 8, 2025
Study Design: Multicenter, randomized, controlled, parallel-group, unmasked trial.
- Included: Low-risk nulliparous women with a singleton, vertex fetus
- Intervention: Elective labor induction between 39+0 days and 39+4 days of gestation.
- Standard Treatment: Expectant Management (participants were instructed to avoid elective delivery before 40+5, and to initiate delivery no later than 42+2)
- N = 6,106 patients from 41 hospitals in the United States, randomized 1:1.
- Intervention Group: N = 3062
- Expectant Management Group: N = 3044
- No specific induction or labor management protocol was mandated in either group.
Primary Outcome: A composite of perinatal death or severe neonatal complications, including one or more of:
- Perinatal death
- Need for respiratory support within 72 hours after birth
- 5 min APGAR < 3
- Hypoxic Ischemic Encephalopathy or Seizure
- Infection (confirmed sepsis or pneumonia)
- Meconium aspiration syndrome
- Birth trauma
- Intracranial or subgaleal hemorrhage
- Hypotension requiring vasopressor support
Secondary Outcomes:
- Cesarean Delivery
- Neonatal birth weight
- Shoulder dystocia
- Operative vaginal delivery
- Chorioamnionitis
- Postpartum Hemorrhage
- Several other maternal and neonatal outcomes listed in the full text
Results: Analyses followed the intention-to-treat principle, with one interim analysis.
Major Outcomes:
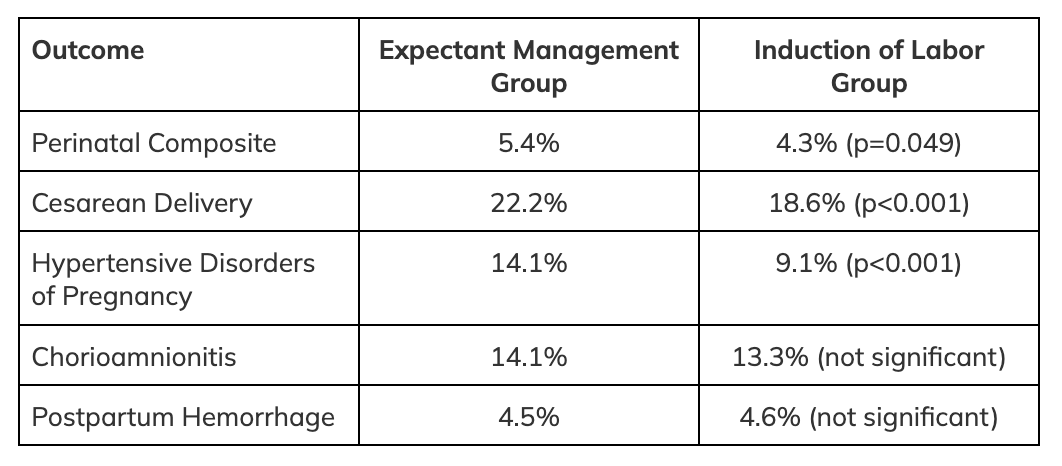
- No significant difference in composite of adverse perinatal outcomes.
- Statistically significant decrease in cesarean delivery rates and hypertensive disorders of pregnancy.
- Neonates in the induction group trended toward shorter respiratory support duration and hospital stays (not statistically significant).
- Mothers in the induction group trended toward more time in the labor and delivery unit (not statistically significant).
Study Pros:
- Randomized Control Trial, large sample size
- Intention-to-treat analysis
Study Cons:
- Results are generalizable to only healthy, nulliparous women
- Sample size too small to detect differences in rare neonatal adverse events
Dr. M's Perspective
The ARRIVE Trial demonstrated that among low-risk nulliparous women with singleton pregnancies, elective induction at 39 weeks did not significantly reduce the composite of adverse perinatal outcomes, but did significantly lower cesarean delivery rates and hypertensive disorders compared to expectant management.
The results of this trial are hardly controversial - it was a well designed study! So what is all the fuss about? The debate around elective inductions seems to center around a generalized feeling that, on a population level, we are not seeing the benefits observed in the study, and may be seeing some adverse events like increased time in labor, intrapartum infections, and negative neonatal outcomes.
The extent to which these observations have been confirmed or refuted by high-quality studies is beyond the scope of this newsletter, but will be discussed thoroughly by Dr. Megan Whitham at OB Shock 2026! Until then, here are a few thoughts on the current state of clinical practice:
- Post-ARRIVE, enthusiastic endorsements by trusted organizations caused clinicians to rapidly, and in some instances, inappropriately adopt and extrapolate the results of the study to populations not included in the original study design. Examples include multiparous patients, and patients who are not truly low risk (eg obese patients).
- Even the best-designed study may show its weaknesses when clinician preferences, skill, and patient factors influence its real-world implementation.
- Professional societies must be measured, unbiased, and responsible in their promotion of study results. It is difficult to un-ring a bell (remember the aggressive promotion of the WOMAN Study?)!
When we see discrepancies between research findings from a study population and observed outcomes in the real world, it is our responsibility to re-evaluate our practices in a rigorous and unbiased manner.
We hope to see you in Houston for a deep dive into elective inductions, and where we go from here!
1. Grobman WA, Rice MM, Reddy UM, Tita ATN, Silver RM, Mallett G, Hill K, Thom EA, El-Sayed YY, Perez-Delboy A, Rouse DJ, Saade GR, Boggess KA, Chauhan SP, Iams JD, Chien EK, Casey BM, Gibbs RS, Srinivas SK, Swamy GK, Simhan HN, Macones GA; Eunice Kennedy Shriver National Institute of Child Health and Human Development Maternal–Fetal Medicine Units Network. Labor Induction versus Expectant Management in Low-Risk Nulliparous Women. N Engl J Med. 2018 Aug 9;379(6):513-523. doi: 10.1056/NEJMoa1800566. PMID: 30089070; PMCID: PMC6186292.